Understanding the Central Nervous System: Immune-Mediated vs. Biomechanical Pathophysiology
1. Introduction: The Two Lenses of Neurological Health
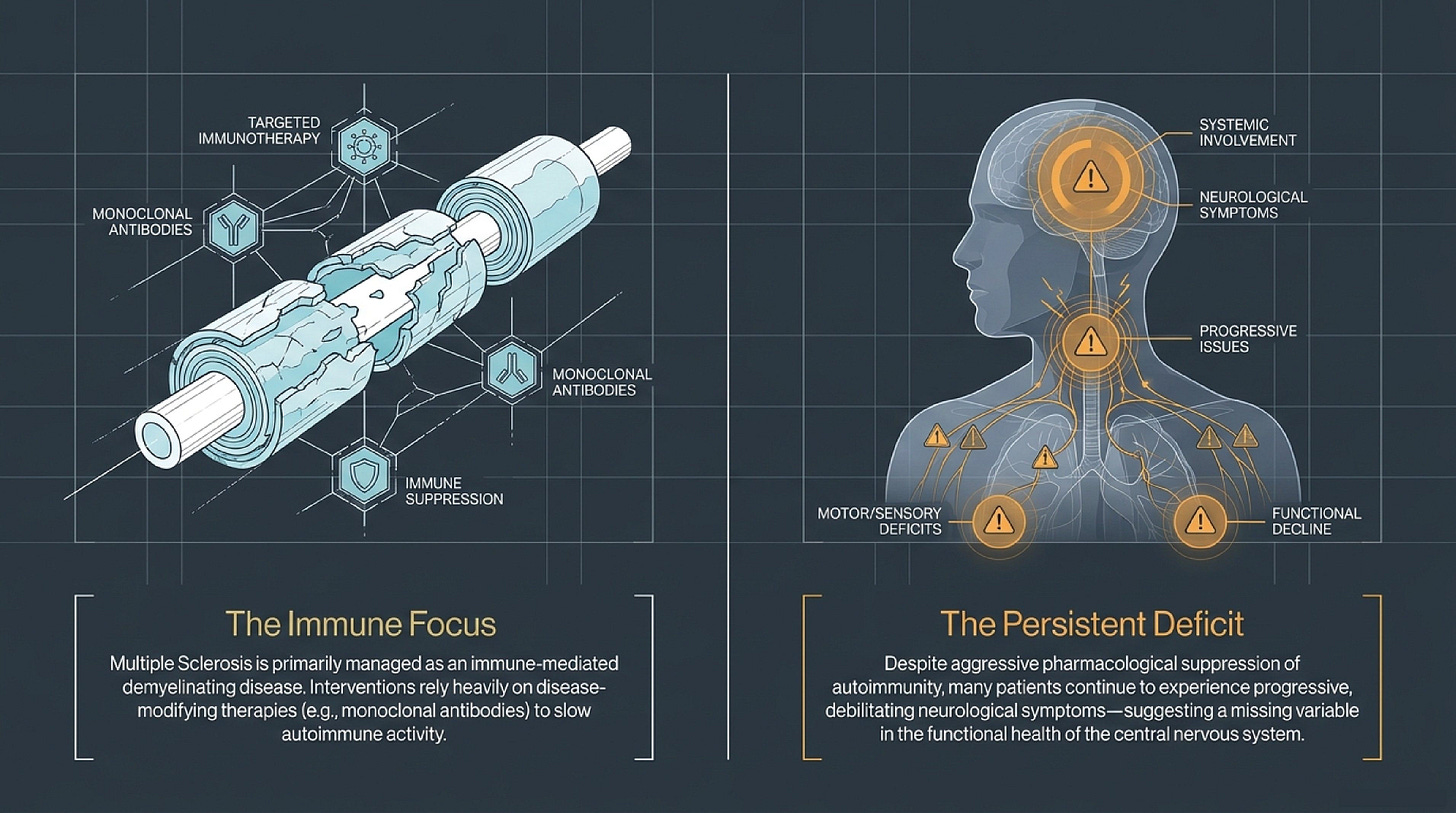
To achieve clinical mastery in the management of complex neurological disorders, we must differentiate between two distinct but interdependent paradigms: the traditional “disease management” model and the emerging “structural environment” model. The former focuses on the cellular-level “attack”—the immunological dysregulation that characterizes conditions like Multiple Sclerosis. The latter examines the “plumbing and wiring” of the central nervous system (CNS), shifting the focus to the neurovascular gateway where spinal architecture dictates physiological function.
These perspectives are not mutually exclusive; rather, they represent different layers of care. While immunotherapy targets the rogue immune “actors,” neuro-biomechanical intervention addresses the “stage”—the physical environment of the spine and skull that must remain patent for the CNS to thrive. Clinical success often hinges on recognizing that even the most advanced medical therapy may struggle if the physical conduit of the nervous system is compromised.
2. The Immune-Mediated Paradigm: Multiple Sclerosis (MS) Defined
Multiple Sclerosis is defined as a chronic, idiopathic, immune-mediated disease of the CNS. The most prevalent phenotype is Relapsing-Remitting Multiple Sclerosis (RRMS), marked by acute episodes of neurological deficit followed by varying degrees of recovery.
As clinicians, we must understand the three primary pathophysiological pillars of the MS “attack”:
Immune Dysregulation: The immune system misidentifies CNS tissues as foreign, initiating a localized inflammatory cascade.
Myelin Damage: The inflammatory response targets the myelin sheath, the lipid-rich insulation of nerve fibers. Demyelination leaves the axon vulnerable and impairs saltatory conduction.
Signal Disruption: The functional consequence is a “short-circuiting” of electrical impulses, resulting in the diverse neurological deficits seen in the patient.
Common Symptoms of RRMS
Profound fatigue and cognitive impairment (”brain fog”)
Vertigo and debilitating dizziness
Paresthesia (numbness, tingling, or “burning” sensations)
Gait instability and ataxia
Visual disturbances
Cervicogenic headaches
While the immune system drives the cellular pathology, the spine and skull provide the structural framework that can either support or hinder neurological recovery.
3. The Biomechanical Paradigm: The Craniocervical Junction (CCJ) & Subluxation
In neuro-biomechanical sciences, we prioritize the Craniocervical Junction (CCJ)—the articulation of the occiput (C0), Atlas (C1), and Axis (C2). This region serves as the “neurovascular gateway,” housing the brainstem, Vertebral Arteries, and the Vertebral Venous Plexus (VVP).
A Vertebral Subluxation in this region is a structural shift that creates mechanical obstruction and environmental stress. We must specifically recognize the Atlas Subluxation Complex (ASC) as a primary driver of neuro-biomechanical interference.
CCJ Function: Structural Comparison
Feature
Normal Structural Function
Subluxated State (ASC)
Alignment
Precise C1/C2 orientation relative to the occipital condyles.
Lateral displacement or rotational misalignment of the Atlas.
Nerve Communication
Unimpeded signaling across the brainstem-spinal cord interface.
Mechanical obstruction of neural pathways and signal interference.
Tissue Stress
Optimal dural tension; minimal mechanical strain on CNS.
Increased mechanical tension on the dura mater and spinal cord.
Postural Impact
Neutral head carriage; healthy cervical lordosis.
Anterior head carriage and Cervical Hypolordosis (loss of curve).
This structural misalignment does more than pinch nerves; it fundamentally alters the “fluidics” and waste-clearance mechanisms of the brain.
4. Deep Dive: Three Neurophysiological Mechanisms of Structural Support
The Finn et al. (2026) case study highlights how structural alignment at the CCJ directly influences the internal environment of the CNS through three specific mechanisms:
Cerebrospinal Fluid (CSF) Dynamics:
Structural Obstruction: Subluxation creates mechanical tension on the dura mater at the foramen magnum.
Physiological Consequence: This impedance alters CSF pulsatility, which is the primary driver of the Glymphatic System. Without proper flow, the brain cannot efficiently clear metabolic waste and inflammatory debris.
Cerebral Venous Outflow:
Structural Obstruction: A misaligned atlas can mechanically compress the Internal Jugular Veins (IJVs) or the Vertebral Venous Plexus (VVP).
Physiological Consequence: This creates Venous Hypertension and congestion, which may compromise the blood-brain barrier and sustain the pro-inflammatory environment surrounding MS plaques.
Neuro-Proprioceptive Integration:
Structural Obstruction: Misalignment causes aberrant afferent signaling from the high density of mechanoreceptors in the upper cervical joints.
Physiological Consequence: This results in a “vestibulocerebellar mismatch,” where the brain receives conflicting data regarding balance, directly causing dizziness, vertigo, and gait instability.
These mechanisms demonstrate that structural correction is a prerequisite for physiological normalization.
5. Comparative Analysis: Managing the Disease vs. Supporting the Environment
Clinical mastery requires an integrated view. Medical immunotherapy targets the cells of the immune system, whereas upper cervical chiropractic care (such as the Atlas Orthogonal technique) targets the conduit of the nervous system. Chiropractic does not replace medical care; it optimizes the structural environment so that the body—and the medical therapy—can function more effectively.
Perspective Comparison
Feature
Immune-Mediated Model (Medical)
Biomechanical Model (Chiropractic)
Primary Goal
Suppress autoimmunity; slow disease progression.
Reduce vertebral subluxation; restore neuro-biomechanical function.
Target of Intervention
B-cell depletion (e.g., Kesimpta/Ofatumumab).
Structural alignment of the CCJ and full spine.
Role of Clinician
Directly manage the inflammatory “attack.”
Remove structural interference to support the “conduit.”
The synergy between these models was clearly demonstrated in recent clinical research, where structural stability catalyzed a recovery that medication alone could not achieve.
6. Clinical Synthesis: The Case of the 30-Year-Old Male
The Finn et al. (2026) case study involves a 30-year-old male with RRMS whose condition was failing to stabilize under medical therapy alone. This case provides a rigorous example of why we must look beyond chemistry to the physical architecture of the spine.
The Path to Improvement
Presentation: The patient exhibited severe fatigue, dizziness, gait instability, and a “constant burning sensation” in the feet.
Structural Findings: Imaging confirmed Atlas Subluxation (ASC), Cervical Hypolordosis, and an active demyelinating lesion at the C4–C5 level.
Intervention: He received precision Atlas Orthogonal (AO) adjustments combined with SOT Pelvic Blocking and Diversified Spinal Adjustments. Notably, during the AO adjustment, the patient reported an immediate sensation of “release” or decompression that resolved the long-standing burning in his feet.
Results: A 72.7% reduction in symptom burden and a 75.8% reduction in fatigue. The patient rated himself as “Very Much Improved.”
Critical Insight from MRI Findings: We must emphasize the temporal relationship of the MRI data. A follow-up MRI in March 2024—conducted while the patient was on Kesimpta but before chiropractic care—showed progression and enlargement of the C4–C5 lesion. However, a subsequent MRI on September 12, 2024—after the addition of chiropractic care—demonstrated regression and a reduction in T2 signal intensity and size of that same lesion. This suggests that by improving the CCJ “plumbing,” we likely reduced the neuro-inflammation or edema that the medication alone was unable to control.
7. Learner Summary: The “Grokking” Checklist
As you transition into clinical practice, use these three key insights to guide your reasoning:
Structure Dictates Biology: The spine is the protector of the CNS. Misalignments create mechanical tension on the dura mater, which physically impedes the fluid dynamics (CSF and venous flow) required for neuro-immunological health.
Cells vs. Conduit: Medical models treat the immune cells; the biomechanical model treats the conduit. Stabilizing the conduit creates the necessary environment for the medical treatment to succeed.
Environmental Optimization: As proven by the regression of the C4–C5 lesion in the Finn et al. study, restoring structural alignment can reduce active neuro-inflammation by facilitating the brain’s natural waste-clearance pathways.
By adopting this interdisciplinary, patient-centered approach, we treat the whole person, ensuring that the nervous system is not just “medicated,” but structurally free to heal and regulate.